See How We Boost Revenue & Cut Costs
Discover how our end-to-end billing solution with AI-powered coding and scribing helps practices boost collections, cut errors, and save big.

End-to-end medical billing solutions for California healthcare providers starting at just 2.49% of monthly collections. Take full control of your revenue cycle with our all-in-one service, including AI-powered coding and scribing at no extra cost. Streamline your operations, boost collections, and cut down on billing errors all while saving thousands.
Our Stats
Practices Served
First-Pass Rate
Avg. A/R Days
Client Retention
Discover how our end-to-end billing solution with AI-powered coding and scribing helps practices boost collections, cut errors, and save big.

You’re not just outsourcing billing — you’re upgrading your entire revenue process.

95 %+ clean-claim / first-pass acceptance keeps money flowing.

No recruiting, training, or software to buy — just a simple % of collections.

We shoulder the paperwork so you spend more time with patients.

Instant claim scrubbing, predictive denial alerts, auto-appeal templates.

Ambient AI captures visits, drafts notes, and suggests codes—saving providers 2+ hours/day.

If we don’t hit a ≥95% first-pass rate or cut AR days by 30%, the fee is waived.

HIPAA-compliant, SOC 2–rated processes plus real-time documentation.

Interactive dashboard shows AR days, denials, payer mix, and cashflow.
We manage the entire revenue cycle — tailored to your specialty, volume, and existing systems.

From charge entry to payment posting, we handle every step of your billing process.

We submit claims within 24 hours and aggressively follow up on unpaid claims to reduce your AR days.

We don’t stop at first denials — we investigate, correct, and appeal with full documentation.

We verify patient eligibility and benefits before services, reducing costly denials.
Did you know AI can streamline billing and speed up payments? Let us help optimize your revenue cycle for faster, error-free claims.

Book a Meeting
A streamlined path from free consult to full-service billing, no downtime, no guesswork.


15-minute discovery call to pinpoint coding gaps, denial trends, and revenue leaks.

Specialty-tuned blueprint—updated fee schedules, edit rules, and payer tactics aligned with your EMR.

We sync with your tech stack, configure workflows, and launch with zero disruption so you start collecting faster, right from Day 1.
Your billing is only as good as the people behind it. Here’s what sets our team apart



Skilled across multiple specialties and payer systems.







A single point of contact who knows your practice and handles communication.


Faster claim scrubbing, smart follow-ups, and fewer human errors.



Live support, transparent updates, and full-service partnership.



Just a team that brings you more revenue, fewer headaches, and peace of mind.

No setup fees.

No long-term contracts.

Book an Appointment
We offer a 98% success rate because of the medical billing process we follow. Our billing process paves the path for improved practice revenue.
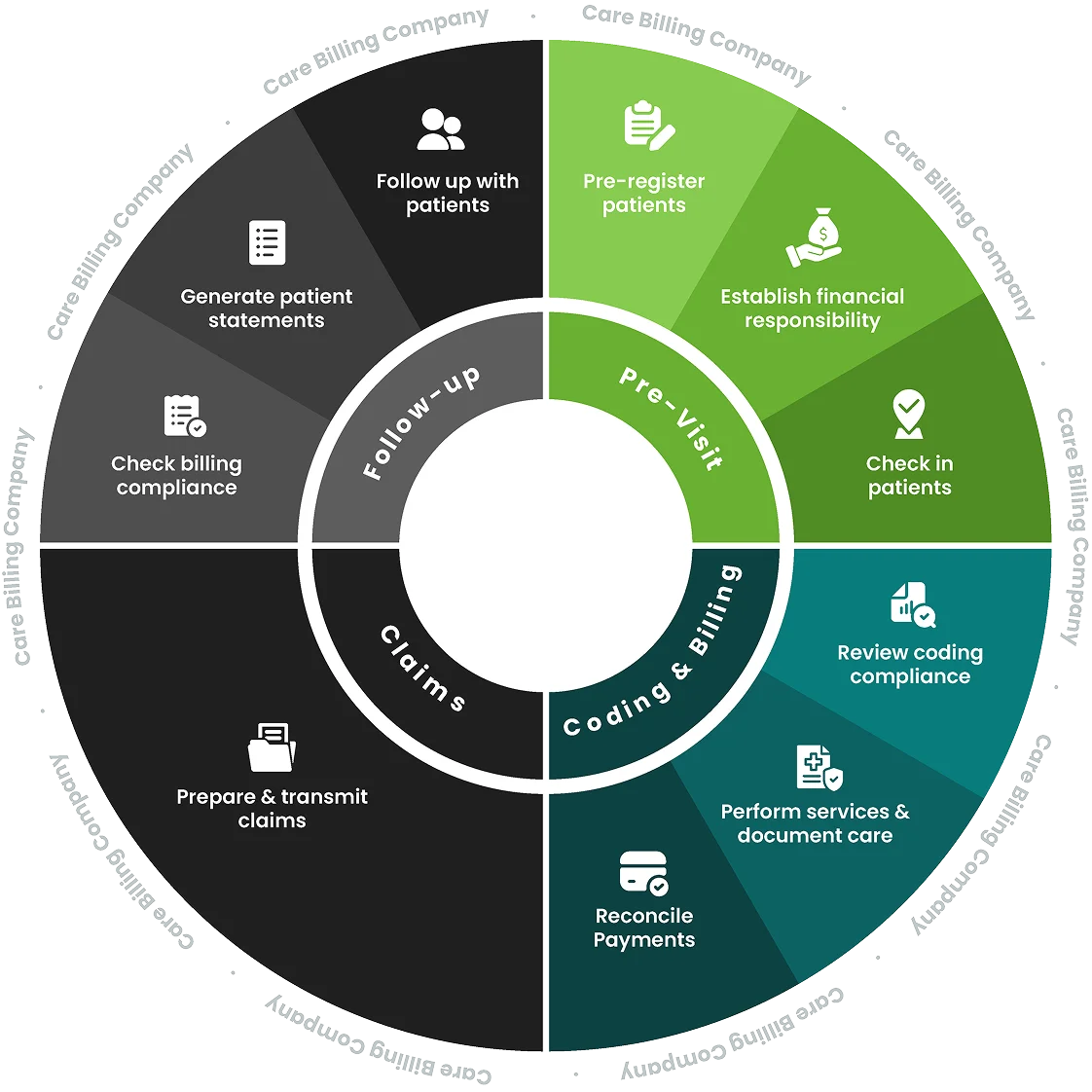
Information gathering and Demographic Entry
Insurance Eligibility and Verification
Medical Coding and Billing
Claim audits and submission
Claim Follow-up and Denial Management
Your billing is only as good as the people behind it. Here’s what sets our team apart

We were losing thousands every month in missed claims and denials. In 3 months, this team turned it around — collections went up 22%.
Dr. Hameed
Family Practice

Their reporting dashboard alone is worth it. I finally understand what’s working, what’s not, and where my money is stuck.
Sarah Lewis
Orthopedic Clinic

They got us credentialed with five payers in record time. Super professional and fast.
David Morales
Practice Owner

Our claim rejection rate dropped significantly, and revenue increased within months. Their team is top-notch and incredibly efficient.
Dr. Emily Johnson
Internal Medicine

Orthopedics

Cardiology

Pediatrics

Anesthesiology

Dermatology

Women’s Health

Mental Health

Radiology

General Surgery

Internal Medicine

Gastroenterology

Neurology

Oncology

Pain Relief

Urology

Urgent Care

Physical Therapy

Dental

Chiropractic

Ophthalmology











